The Invisible Threat
Written by Minjae Yoo
Edited by Sameeha Salman
Jan 31, 2021
Edited by Sameeha Salman
Jan 31, 2021
With COVID-19 headlines dominating the spotlight, you may have heard of the term “asymptomatic carrier”. But what exactly does this phrase mean, and what implications does it have on how we approach the novel coronavirus?
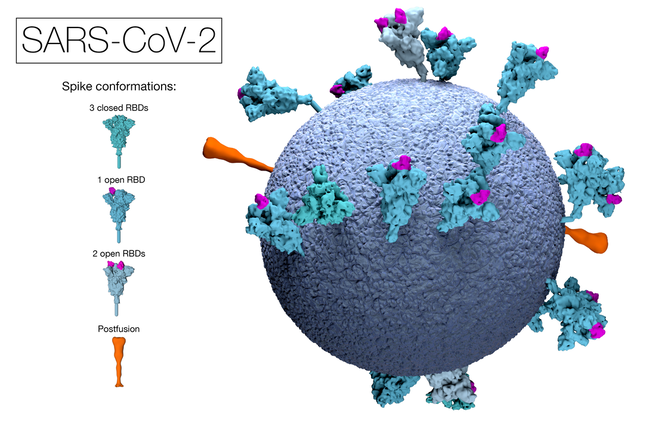
The current pandemic has forced many into a state of fear that they or their loved ones may be at risk of receiving the virus from someone else. Adding to this fear, the U.S. Center for Disease Control and Prevention has recently estimated that a striking 40% of infections are “asymptomatic”. This means that a sizable portion of the U.S. population may be carriers—people capable of disease transmission—despite not experiencing many of the most common symptoms that are indicative of the virus. SARS-CoV-2 (the name of the viral particle that causes COVID-19) is not the first nor only virus to have such asymptomatic carriers. The exact method by which SARS-CoV-2 causes these asymptomatic cases, however, has only recently been uncovered.
Earlier this year, researchers at the University of Arizona discovered that SARS-CoV-2 interferes with our bodies’ abilities to feel physical pain by attaching to receptors of cells in the nervous system called neuropilin-1, or NRP-1. You can think of these receptors as cellular “inboxes” where cells normally receive messages from other cells. The receptors are responsible for transmitting pain messages to the brain, where they are ultimately “felt”.
Viruses are often referred to as obligate intracellular parasites, which just means they need to reside within the cells of another living being in order to survive. Upon entry into the body, viruses attach to the receptors of their host’s cells, entering into and using the biological tools within those cells to make copies of themselves which are then spread rapidly throughout the body, causing an infection.
Under normal circumstances, cells with NRP-1 receive a protein (the “message”) called vascular endothelial growth factor A or VEGF-A, encoded with a pain signal, and re-send it as another message up the chain of command. However, when SARS-CoV-2 enters the scene, one of its own viral proteins attaches to NRP-1 in place of VEGF-A, effectively preventing NRP-1 from performing its role and disrupting the process as a whole. The end result? Those affected by this condition are less likely to feel pain. The team at the University of Arizona believe that this is directly related to certain patients’ failure to experience sore throat, headaches, muscle aches, and many of the other common pain-associated COVID-19 symptoms.
Although this finding suggests we remain evermore vigilant of the virus—regardless of whether the symptoms have manifested—it has also opened up gateways for new scientific research, according to Dr. Rajesh Khanna of the UoA research team. In addition to continuing their study of the pandemic, UoA will be looking at NRP-1 as a site for new, opioid-free pain relief methods in the future.
Works Cited
University of Arizona Health Sciences. "Pain relief caused by SARS-CoV-2 infection may help explain COVID-19 spread." ScienceDaily. ScienceDaily, 1 October 2020. <www.sciencedaily.com/releases/2020/10/201001155912.htm>
“Neuropilin-1.” UniProt ConsortiumEuropean Bioinformatics InstituteProtein Information ResourceSIB Swiss Institute of Bioinformatics. UniProt, 4 Oct. 2018. <www.uniprot.org/uniprot/O14786>
Image Source: "3D model of SARS-CoV-2" by MRC Laboratory of Molecular Biology licensed under CC-BY-NC-ND 4.0