Fixing Cancer Treatments: Can Scientists Bypass a Broken Immune Response?
Written by Daria Beniakoff
Edited by Aryss Hearne
Jan 31, 2021
Edited by Aryss Hearne
Jan 31, 2021
Immunotherapy is an effective cancer treatment, but some patients develop resistance to it. What can scientists do when immunotherapies become ineffective?
Immunotherapy involves stimulating the immune system, inciting it to attack cancer cells. Interferons (IFN) are an important part of an immunotherapy called T-cell based adoptive cell therapy (ACT). IFNs are a group of signaling proteins usually made by cells in response to viruses. Not only can IFNs identify and alarm the immune system about the presence of viruses, but they can also warn the body about cancer cells! So, with the help of functioning IFNs, an oncologist can utilize T-cell based ACT to recruit a cancer patient’s own T-cells to recognize and kill that patient’s cancer cells. While T-cell based ACT is often an effective treatment for certain cancers, the cancer cells’ IFN signals can malfunction, rendering the therapy ineffective. That is, the T-cells need IFNs to help them detect the cancer cells. So, what can scientists do when immunotherapies become ineffective? This is the question Kalbasi et al. sought to answer.
Kalbasi et al. explores how ACT therapy could still be useful for patients with melanoma, a type of skin cancer. Using a mouse model, they discovered cells with defective IFN signaling pathways can still be sensitized to ACT therapy. In order to do so, there needs to be a way to activate the pathway (the now defunct) IFNs would ordinarily trigger. IFNs usually activate a signaling cascade leading to major histocompatibility complex I (MHC I) protein expression. MHC I proteins show specific segments of proteins from viruses and other antigens to T-cells. If the T-cells, which are specialized to react to specific protein fragments, recognize the segment as the one they target, the immune system will activate and the T-cells will start killing the cancer cells. Kalbasi et al. shows that MHC I protein expression can be produced by inducing NLRC5 receptor overexpression through genetic modification. MHC I production can also be induced by introducing BO-112, a lab-produced double stranded RNA (dsRNA), to activate (dsRNA) sensors. Both methods activated alternative pathways that resulted in enough MHC I production to restore the effectiveness of ACT cancer therapy in the mouse model.
Immunotherapy, including ACT therapy, is still an effective treatment for cancer; however, some patients do develop resistance to it through developing defects in IFN signaling. Kalbasi et al. explored how ACT therapy could still be used, as long as there is another way to activate MHC I protein expression. Although this is a preliminary study, it’s findings could be useful in maximizing the effectiveness of ACT therapy for more cancer patients. It also provides a better understanding of alternative pathways to activating the immune system that can be utilized in immunotherapy.
Works Cited
Kalbasi, Anusha, et al. “Uncoupling Interferon Signaling and Antigen Presentation to Overcome Immunotherapy Resistance Due to JAK1 Loss in Melanoma.” Science Translational Medicine, American Association for the Advancement of Science, 14 Oct. 2020, stm.sciencemag.org/content/12/565/eabb0152.
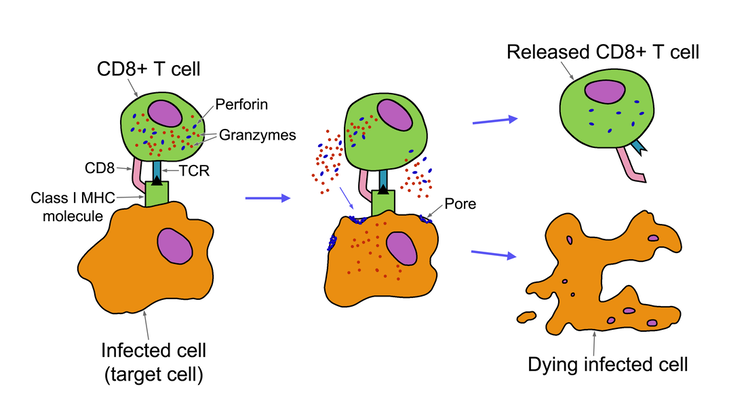
Image Source: "Mechanism of CD8+ T cell destruction of infected cells" by Dana Nguyen licensed under CC BY-SA 4.0